The world has never seen anything like the race for Covid-19 vaccines. The breadth and speed of the effort is astonishing, with more than 160 projects underway, by World Health Organization counts. “All the strategies that have ever been used to make a vaccine, as well as several new strategies, are being used to make this one,” says Paul Offit, a pediatrician and vaccine developer at the Children’s Hospital of Philadelphia.
Vaccine development usually takes more than a decade, but in this case the first large clinical trials have already begun or are being launched. If these phase 3 trials, as they’re termed, provide enough evidence of effectiveness, emergency regulatory approvals could soon follow.
But vaccine development is famously tough. Despite the unprecedented speed, preliminary results from the earliest trials are only starting to trickle in, says microbiologist and infectious disease specialist Maria Elena Bottazzi of Baylor College of Medicine, who is a co-lead developer of a Covid-19 vaccine and coauthor of an article about vaccines for developing countries in the Annual Review of Medicine.
And though the SARS-CoV-2 virus causing the pandemic is being intensively studied in thousands of labs, it retains many mysteries that may affect vaccine safety and effectiveness.
How are Covid-19 vaccines being developed, tested and readied for approval? How will their safety and effectiveness be assessed — in a time when many people view vaccines with suspicion? Here’s a quick guide.
How does developing vaccines for Covid-19 differ from normal drug development?
Speed. These are all-out efforts to develop the vaccines in record time, while still following all the steps necessary to assure their safety.
Each vaccine developer essentially has put its eggs into one or two baskets rather than having 20 varieties to test in the lab or in animals, says Manish Sadarangani, head of the Vaccines Evaluation Centre at BC Children’s Hospital in Vancouver, Canada, which pursues many forms of Covid-19 research.
Regulators also have sped up the administrative process, prioritizing Covid-19 vaccines and reducing paperwork without compromising safety, Sadarangani says. And they’ve allowed some shortcuts to hasten clinical studies. For instance, the company Moderna Therapeutics, whose Covid-19 vaccine candidate (co-developed with the National Institute of Allergy and Infectious Diseases) was the first to run an early (phase 1) safety trial in the United States, was permitted to run the trial in parallel with full animal testing.
Recruiting volunteers for these trials hasn’t been a problem: People are keen to participate, Sadarangani says. Professionals working on the trials, such as statisticians analyzing data and physicians on independent safety monitoring committees, give them top priority. “People are willing to work around the clock,” Sadarangani says.
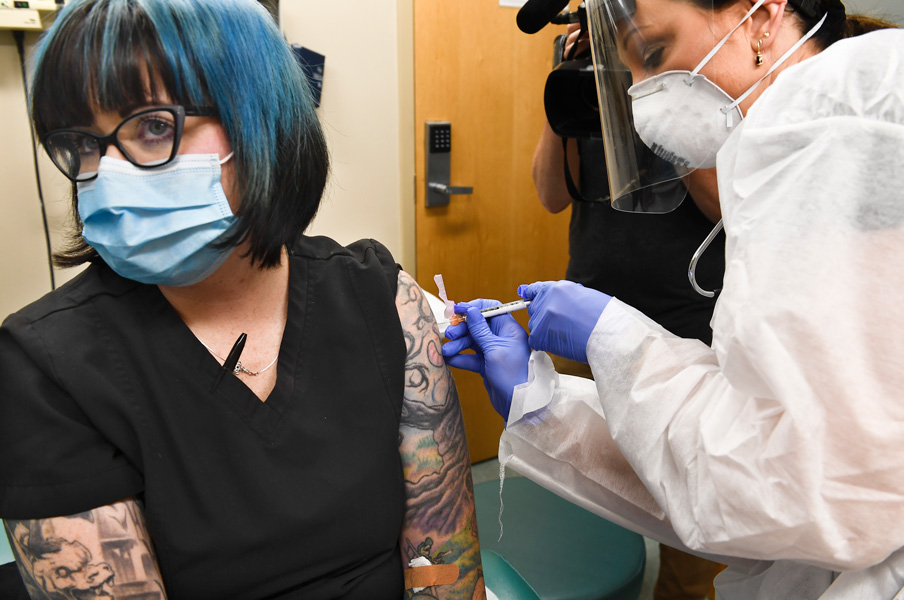
A volunteer in Binghamton, New York, receives an injection of a Covid-19 candidate vaccine in a newly launched phase 3 clinical trial. Developed by Moderna, Inc. and the National Institutes of Health, it is one of several vaccines now in large-scale testing.
CREDIT: AP PHOTO / HANS PENNINK
What does the safety record look like for other vaccines that have been developed?
Good. “Vaccine developers are probably more concerned with safety than any other aspect of vaccine performance,” says Terence Dermody, a pediatrician and virologist at the University of Pittsburgh. “Because, quite frankly, if the vaccine is not safe, it doesn’t matter if it induces an immune response and it protects you.” Vaccines are given broadly and to people who are healthy, so even a small risk is unacceptable.
Vaccines for diseases ranging from flu to measles to pneumococcal infections have a solid record of safety. While some people worry about the risk of anaphylactic shock (a life-threatening immune reaction), that’s about a one-in-a-million chance with most vaccines, Sadarangani says.
The two polio vaccines, Salk and Sabin, offer another example of issues involving safety, Dermody adds. Both vaccines are extremely effective, but they differ: The Salk consists of fully destroyed virus while the Sabin is live virus that has been rendered harmless — attenuated. But there is a one-in-a-million (or lower) chance that the attenuated virus will mutate and flip back to a disease-causing state, causing polio cases. For that reason, the Sabin vaccine is not used in the US.
One vaccine that’s often cited as a counterexample is a dengue vaccine that killed several young Filipino children. But the dengue outcome was unusual, driven by a phenomenon known as antibody-dependent enhancement, in which antibodies triggered by exposure to a pathogen or vaccine actually help the pathogen get into cells. Dengue comes in several strains and the vaccine does not protect equally against all of them; the deaths occurred in children who had not been exposed to dengue before, and later encountered a strain that the vaccine didn’t protect against.
For this reason, the vaccine never got a thumbs-up for such children from the US Food and Drug Administration, and the WHO now recommends it only for individuals who have had dengue in the past.
What makes SARS-CoV-2 a particular challenge for vaccine researchers?
“It’s an unusual virus that we’re still learning about,” Offit says. Scientists don’t really know how the human immune system beats it back. Among the puzzles: Some people who develop symptoms don’t seem to generate much of an immune response, while others may kick off life-threatening immune overreactions called cytokine storms. Such overreactions have been seen in other diseases, including two caused by coronaviruses related to the one behind Covid-19: severe acute respiratory syndrome (SARS), which broke out in 2003, and Middle East respiratory syndrome (MERS), first reported in 2012.
There are worries, in fact, that Covid-19 vaccines themselves may ignite immune over-responses. “That’s really an open question right now,” says Stanley Perlman, a virologist at the University of Iowa and a coauthor of an article about the MERS virus in the Annual Review of Medicine.
No vaccines were ever approved for SARS or MERS, though vaccine candidates entered early clinical studies: Both diseases were stamped out mostly by testing and isolating infected people. But several of the Covid-19 candidates have built on the SARS and MERS vaccine work, offering important clues on effectiveness and safety. Both immune overreactions and antibody-dependent enhancement cropped up in animal studies of SARS vaccine candidates, and developers are on the lookout for both risks as they design and test their candidates.
Will the manufacturing method influence the likelihood of agencies granting emergency approval for Covid-19 vaccines?
Clinical trials will be used to provide evidence of safety and effectiveness, regardless of the precise technique by which a vaccine is made.
Developers are taking a wide range of approaches and they don’t know which one is most likely to work. For instance, among the candidates now in phase 3 trials, vaccines from China’s Sinopharm and a collaboration between the University of Oxford and the company AstraZeneca use a non-replicating virus — a harmless virus particle that can’t reproduce but carries genetic material encoding the SARS-CoV-2 spike protein. The Chinese biotech company Sinovac uses inactivated — killed — Covid-19 virus.

Brazil's João Doria, Governor of São Paulo, holds a sample of a candidate vaccine at a July 21 press conference. The vaccine, from the Chinese pharmaceutical company Sinovac, is now in large-scale clinical trials in Brazil.
CREDIT: SIPA USA VIA AP IMAGES
The Moderna vaccine is based on messenger RNA molecules that contain instructions for making SARS-CoV-2 proteins. Once the mRNA is injected, the recipient’s own cells generate the vaccine proteins. This is a new approach that has shown promise in small, early clinical trials for SARS-CoV-2 vaccines and ones against other viruses, but no mRNA-based vaccine has yet been approved for any infectious disease.
These varied approaches raise different challenges in designing, manufacturing and delivering a vaccine, but regulatory agencies will monitor each step for safety and effectiveness.
How are the phase 3 clinical studies designed?
The WHO, the FDA and other regulatory bodies are setting up common guidelines for these crucial big trials so that vaccines can be judged systematically.
Typically, the main measurement for approval is prevention of Covid-19 disease with detectable symptoms. The trials all need to run until tests show that a certain number of participants have been exposed to the virus in their normal lives. (So far, no trials have been approved that directly expose healthy participants to the Covid-19 virus, although such human challenge trials have been discussed.)
Thousands of people need to be enrolled to see results. For example, among the first phase 3 studies — all of which followed earlier, smaller studies — a trial of Moderna’s vaccine candidate will enroll about 30,000 healthy people in the US and give half of them the vaccine candidate. The other half — randomly selected — will get a placebo. And the University of Oxford/AstraZeneca collaboration plans to test its vaccine in roughly 50,000 people in the United Kingdom and several other countries.
By the time you look at this, it may be out of date — that’s how fast Covid-19 vaccine research is moving. Above are candidate vaccines that, as of July 30, have passed through safety trials and entered large clinical trials in which tens of thousands of volunteers will receive — on a random basis — the experimental vaccine or a sham. Then it’s a matter of tracking to see if the vaccine group is better protected against Covid-19 circulating in the community than the control group. Safety monitoring is a key part of such trials. A broad array of vaccine approaches is being looked at — in the six above, three vaccines use killed (inactivated) virus particles. One vaccine uses a harmless virus that causes colds in non-human primates; it cannot replicate in human cells and has been modified so that it directs the manufacture of the spike protein that sits on the surface of the SARS-CoV-2 virus. Two use messenger RNA that carries instructions for a version of the SARS-CoV-2 spike protein. The RNA is encased in an oily lipid envelope to help it enter cells; once inside, the cell’s protein-making machinery creates the spike protein, which can’t cause disease but enables the immune system to be primed for a later encounter with the SARS-CoV-2 virus itself.
What will these studies tell us about the vaccine’s safety?
The trials will be large enough to pick up short-term and common safety problems, Dermody says. “If one in 30 people develop high-grade fever or a seizure, you’ll see that.”
Side effects that take longer to develop or are very rare — affecting, say, one in 10,000 or 100,000 people — will be harder to spot, Dermody adds. But “I have confidence that even with the warp speed magnitude of this work, these study subjects will be observed very carefully,” he says.
Additionally, the United States and most other high-income countries have systems in place to pick up very rare but potentially serious adverse events from vaccines after they have been approved and are given to vast numbers of people beyond clinical trials.
What side effects will be seen as acceptable in a vaccine proposed for wide adoption?
Some side effects are not acceptable in terms of medical harm — even fainting, as experienced by a healthy 29-year-old volunteer who was given the highest test dose of the Moderna vaccine. That dose was dropped from further testing.
Others are more benign. “People may get sore arms and swelling and fever, and some of these vaccines may cause more of those side effects than some of the vaccines we use routinely,” Sadarangani says. A vaccine under development by CanSino Biologics, for example, produced fever in almost half of its recipients in an early trial.
But in a pandemic, these reactions might be acceptable to many, particularly if someone is in a high-risk group. And they might be similar to those for a number of existing vaccines. For example, about one in six people given the Shingrex shingles vaccine have side effects such as headache or muscle pain that interfere with normal activities for a few days, according to the Centers for Disease Control and Prevention.
How effective must vaccines be?
“Vaccine developers are probably more concerned with safety than any other aspect of vaccine performance ….If the vaccine is not safe, it doesn't matter if it induces an immune response and it protects you.”
Both the WHO and the FDA say they will require at least 50 percent effectiveness for a full Covid-19 vaccine approval, and the WHO lists at least 70 percent effectiveness as a preferred goal. (For comparison, two doses of the measles/mumps/rubella vaccine offer about 97 percent protection to children, while the effectiveness of last season’s annual flu vaccines was about 45 percent in the US.) Though neither agency has a detailed definition of “effectiveness,” the ability to prevent severe disease is key. The FDA and other regulatory agencies also can authorize emergency use for vaccines that don’t meet these standards, on a case-by-case basis.
How much control over the pandemic we would get from this level of effectiveness also depends, of course, on how widely vaccines are adopted. There are no magic numbers, says Michael Osterholm, an infectious disease expert at the University of Minnesota at Minneapolis. “Anything we get will be helpful.”
If a vaccine is effective, will it prevent recipients from transmitting Covid-19?
Not necessarily. The FDA may consider a vaccine effective if recipients end up with a mild case of the disease or carry the virus without getting sick at all. In such a case, Perlman says, there is a possibility we might be protected ourselves but potentially still shed the virus to people who haven’t been vaccinated, although maybe dramatically less than an infected person would.
How long will the trials run?
Solid answers might come as quickly as three to five months after full enrollment in a phase 3 trial, the WHO says. Experts cautiously concur, but setting exact deadlines for these trials isn’t possible. Since the trials require enough people who got the vaccine or placebo to be exposed to the virus in daily life, results may come sooner in spots where the pandemic is raging, and later in places where it’s less severe.
Do experts worry that vaccines will be licensed prematurely?
Yes. They see a risk that regulatory agencies will be pressured from above to give green lights to products before proper, careful trials have fully run their course. “Regulatory bodies know how to be very cautious at reviewing the data and allowing the stages to proceed, and there are a lot of other checks and balances in place,” Bottazzi says. “We know that the process works. I hope that they don’t feel that they need to jump over some of the process in the safety arena because they need something quick.”
Offit and a coauthor warned of just such a dangerous scenario in the US in a June opinion article in the New York Times. “Obviously, when we have a thousand people dying a day, we want to get something out there as quickly as possible to save people’s lives,” he says now. “But we certainly should do this the way we’ve always done: with large placebo-controlled phase 3 trials. We can’t short-circuit that step, because that’s the proof.”
When and if vaccines prove safe and effective, how will the public view them?
Broad adoption will be a struggle in many countries, even if trials deliver solid clinical proof.
A May 2020 survey in the United States, for example, found that only 49 percent of the 1,056 respondents said they planned to get a Covid-19 vaccine. (Other polls have reported higher numbers.) “If we start getting vaccines that don’t work and have side effects, that 49 percent, which is really horrible, will go even lower,” Perlman says. “On the other hand, if we have evidence that a vaccine is working, I think the 49 percent could creep up to the maximum, which is probably around 85 percent in the US. It’s really important that this be done right.”
A minority of people are so opposed to vaccines they will never accept them as safe, but “most people trust vaccines,” Offit says. “We need to make sure that as we move forward with these vaccines, we manage expectations so that we don’t lose the confidence of the American public.”
Readiness to take a vaccine presumably will grow as the Covid-19 toll keeps climbing. “I don’t think people have a good sense of just how much more pain, suffering, death and economic disruption still will occur,” Osterholm says. “It’s a crazy situation right now. We’ve just got to stay with the science.”
This article is part of Reset: The Science of Crisis & Recovery, an ongoing series exploring how the world is navigating the coronavirus pandemic, its consequences and the way forward. Reset is supported by a grant from the Alfred P. Sloan Foundation.




